Surgery Overview
Coronary artery bypass is surgery to treat coronary artery disease. It helps blood make a detour, or bypass, around one or more narrowed or blocked coronary arteries. These arteries are the blood vessels that bring blood to the heart muscle. This is also called coronary artery bypass graft (CABG) or bypass surgery.
Your doctor will make the bypass with a healthy piece of blood vessel from another part of your body. Then the doctor will attach, or graft, the healthy blood vessel to the narrowed or blocked artery. The new blood vessel bypasses the diseased artery to increase blood flow to the heart muscle.
The doctor typically makes a cut in the skin over your breastbone (sternum). This cut is called an incision. Then the doctor will cut through your sternum to reach your heart and coronary arteries. The doctor may connect you to a heart-lung bypass machine. It adds oxygen to the blood and moves the blood through the body. The machine will allow the doctor to stop your heartbeat while working on your arteries. The doctor will use blood vessels from your chest, arm, or leg to bypass the narrowed or blocked parts of your arteries. When the blood vessels are in place, the doctor will restart your heart. In some cases, the doctor may be able to do the surgery without using a heart-lung machine. This is called "off-pump" surgery.
The doctor may use wire to put your sternum back together. Stitches or staples will be used to close the incisions in the skin over your sternum and where your healthy blood vessel was taken. The wire will stay in your chest. The incisions will leave scars. They may fade with time.
You will stay in the hospital for a few days after surgery. You will probably be able to do many of your usual activities after 4 to 6 weeks. But for at least 6 weeks you will avoid lifting heavy objects and doing things that strain your chest or upper arm muscles. At first you may notice that you get tired quickly. You may need to rest often. It may take 1 to 2 months before your energy is back to normal.
How It Is Done
A coronary artery is narrowed or blocked
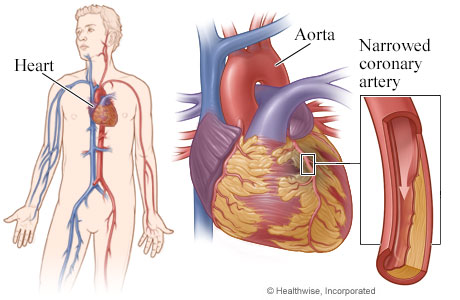
Coronary artery bypass grafting (CABG) surgery reroutes blood around narrowed or blocked arteries, increasing blood flow to the heart muscle tissue.
Incision in the middle of the chest for open-heart surgery
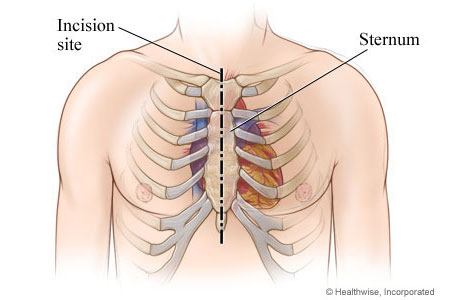
Bypass surgery is most often done as an open-heart surgery. The surgeon makes a vertical incision in the skin and muscle in the middle of the chest and then cuts through the breastbone (sternum).
The heart is exposed
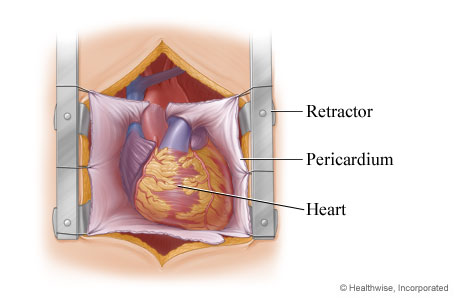
The surgeon spreads the rib cage with a retractor to expose the heart and then cuts through the lining that protects the heart (pericardium).
Blood flow is rerouted
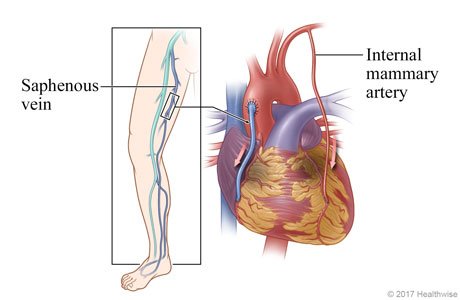
To reroute blood flow around the diseased blood vessel, surgeons use a blood vessel taken from another part of your body. For example, the saphenous vein from the leg or an internal mammary artery from the chest may be used.
Oxygen-rich blood flows to heart muscle
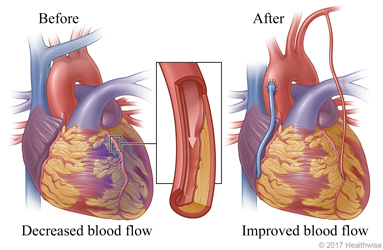
Regardless of which type of blood vessel is used, oxygen-rich blood from the aorta is rerouted around the narrowed or blocked section of the coronary artery to improve blood flow to the heart muscle.
What To Expect
Right after surgery
You will go to the intensive care unit (ICU) after surgery. You will probably stay in the ICU for 1 or 2 days before you go to your regular hospital room. In the ICU, you will likely have:
- Continuous monitoring of your heart.
- A tube to help with breathing for up to a few hours.
- A stomach tube that removes stomach secretions until you start to eat again.
- A tube (catheter) to drain the bladder and measure urine output.
- I.V. tubes in your arms to get fluids, nutrition, and medicine.
- A thin tube in a vein in your neck that keeps track of your heart.
- A thin tube in a blood vessel in your arm to measure blood pressure.
- Several thin wires coming out of your chest. These help keep your heartbeat steady.
- Chest tubes. These tubes drain the chest cavity of fluid and blood (which is temporary and normal) after surgery.
Recovery
You will stay in the hospital for at least a few days after the surgery. You will feel tired and sore for the first few weeks. Your chest, shoulders, and upper back may ache. These symptoms usually get better in 4 to 6 weeks. It may take 1 to 2 months before your energy level is back to normal. You may have some swelling or pain in the area where the healthy blood vessel was taken.
You will probably be able to do many of your usual activities after 4 to 6 weeks. But for at least 6 weeks, you'll avoid lifting heavy objects and doing activities that strain your chest or upper arm muscles.
After surgery, have a heart-healthy lifestyle. This lifestyle can help lower your risk of a heart attack or stroke. It also can help the bypass last as long as possible. To have a heart-healthy lifestyle:
- Take your medicines.
- Do not smoke.
- Eat a heart-healthy diet.
- Get regular exercise.
- Stay at a healthy weight or lose weight if you need to.
- Manage other health problems such as diabetes, high blood pressure, and high cholesterol.
Smoking can make it harder for you to recover. It will raise the chances of your arteries getting narrowed or blocked again. If you need help quitting, talk to your doctor about stop-smoking programs and medicines. These can increase your chances of quitting for good.
You may start a cardiac rehabilitation (rehab) program in the hospital. This program will continue after you go home. It will help you recover. And it can prevent future problems with your heart. Talk to your doctor about whether rehab is right for you.
Learn more
Why It Is Done
Bypass surgery is done to treat a heart attack and coronary artery disease. Surgery might be an option for many reasons. These reasons include the following:footnote 1
- Your left main heart artery is very narrow.
- Multiple arteries of the heart are blocked or the amount of blood flowing through them is very low.
- You are going to have surgery to repair or replace a heart valve.
- You have diabetes and two or more narrowed or blocked arteries.
- Your heart is having trouble pumping. This is called a decreased ejection fraction.
Whether surgery is an option for you also depends on your age, your health, and how much your angina is affecting your quality of life. Your doctor is likely to recommend bypass surgery only if you will benefit from it and if those benefits are greater than the risks. You and your doctor can work together to decide if you want to have surgery.
Learn more
How Well It Works
Bypass surgery:
- Can relieve stable angina symptoms and improve quality of life. You may be able to do more of your daily activities.footnote 2
- May help certain people who have stable angina live longer. Whether it might help you live longer depends on several things. These include your overall health and which arteries need to be bypassed. For example, the surgery may raise your chances of living longer if you have diabetes and narrowing in your heart's larger arteries.footnote 1
- Improves blood flow to the heart muscle after a heart attack.
Risks
The risks during or soon after bypass surgery include:
- Infection.
- Kidney problems.
- Atrial fibrillation.
- Heart attack.
- Stroke.
- Short-term problems with thinking and memory. This is more common in older people. It tends to get better within several months of surgery.
- Death.
The chances of having a serious problem with bypass surgery increase with age. Your risk is also higher if you have other problems such as diabetes, kidney disease, lung disease, or peripheral arterial disease. Your doctor can help you understand what your risk for problems is.
References
Citations
- Lawton JS, et al. (2022). 2021 ACC/AHA/SCAI Guideline for coronary artery revascularization: A report from the American College of Cardiology/American Heart Association. Journal of the American College of Cardiology, 79(2): e21–e129. DOI: 10.1016/j.jacc.2021.09.006. Accessed December 9, 2021.
- Bravata DM, et al. (2007). Systematic review: The comparative effectiveness of percutaneous coronary interventions and coronary artery bypass graft surgery. Annals of Internal Medicine, 147(10): 703–716.
Credits
Current as of: October 2, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: October 2, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.